Occupational therapy and neuromuscular diseases: key support to promote autonomy
The occupational therapist is a health professional who evaluates a person’s autonomy in their daily life activities; namely their abilities and possible limitations. When there is a mobility deficit, it can concern strength, grasping, coordination, etc. (A mobility deficit may result in lack of strength, altered grasp, coordination, etc.)
Once the difficulties in daily activities and the rehabilitation objectives of the person are identified, the neuromuscular occupational therapist proposes personalized rehabilitation and adaptation methods. This may involve functional rehabilitation exercises or appropriate compensatory means (technical aids, wheelchair, etc.). The objective is to allow the person living with a neuromuscular deficit to maintain some autonomy both at home and during mobility.
Content reviewed and approved by Théo Lambert and Océane Arnaud, french occupational therapists

What is neuromuscular occupational therapy?
Definition and role of the occupational therapist
Occupational therapy is a paramedical profession whose practice revolves around autonomy, whether maintaining it, regaining it, or improving it. The neuromuscular occupational therapist supports people with motor deficits that limit the performance of daily tasks, leading to decreased autonomy and independence.
During a session with the neuromuscular occupational therapist, he/she takes the time to get to know the person, their environment (human and material), and their specific needs. They primarily consider the activities that are meaningful to the person. They assess the difficulties encountered in daily life and propose compensatory means to facilitate everyday actions. This involves adapting the environment, learning compensatory movements, setting up appropriate technical aids, etc.
Why do neuromuscular diseases require a specialized approach?
Neuromuscular diseases include a set of pathologies that affect the muscles and nerves responsible for movement. Depending on the pathology, symptoms may appear progressively: muscle tone deficit, loss of strength, coordination disorder, grasp deficit, fatigability, appearance of pain, etc. All this progression contributes to a greater or lesser loss of autonomy, and this is where occupational therapists intervene.
- They assess specific needs according to the progression of the disease.
- They facilitate access to the environment and secure mobility by recommending adaptations.
- They adjust the equipment used: wheelchairs, posture adaptations, grasping tools, etc.
- They implement functional neuromuscular rehabilitation sessions, to maintain remaining capacities and teach new compensatory movements
The objective of these measures is to delay as much as possible the total or partial loss of autonomy.
Daily challenges of people living with neuromuscular diseases
Common difficulties encountered
Neuromuscular deficits can affect certain tasks such as:
- Dressing
- Eating
- Using a computer
- Walking
- Washing
- Using a phone
- Standing up (from a chair or bed)
Etc.
This results in muscle fatigue, hence the need for specific ergonomic adaptations to these difficulties.
Importance of early care
The earlier the intervention of an occupational therapist, the more effective the adaptation of the environment and equipment. This way, the health professional can better preserve the autonomy ofthe person with a disability and prevent possible future complications.
For occupational therapist D.E Christophe Prudhomme (CHU d’Estaing, Clermont-Ferrand), a preventive approach is needed. For him, it is crucial to act quickly to preserve the child’s functional abilities: “The advantage in pediatrics compared to adults is that in children, the function has not been lost for long (or is not completely gone), so it is easier.”

Approaches in occupational therapy for neuromuscular diseases
Adaptation of movements and optimization of posture
In neuromuscular diseases, occupational therapy plays a key role in maintaining quality of life and autonomy of the people concerned. The main objective is to reduce muscle fatigue and preserve a certain range of motion possible with or without assistance. Occupational therapists therefore implement compensation and fatigue prevention techniques such as: simplification of movements, alternating activity and rest, adjusting work positions, or integrating appropriate technical aids.
Examples of solutions set up by an occupational therapist (non-exhaustive list):
- Arm supports
- Orthoses
- Ergonomic cushions
- Adapted wheelchairs
- Ergonomic canes
The health professional provides a personalized approach to equipment by targeting deficits induced by neuromuscular disorders. He/she allows the person with a disability to find the “right fit” for their environment and lifestyle.
Tools and technical aids for daily life
Recommended, tested, or even custom-made, technical aids are central in occupational therapy support. They help significantly improve daily quality of life and promote autonomy:
- Grasp assistance devices: ergonomic pens and adapted cutlery.
➡️ Compensate muscle weakness and preserve autonomy in daily gestures. - Motorized assistance solutions: electric wheelchairs and robotic arms.
➡️ Facilitate mobility and actions requiring range or strength the person can no longer provide alone
Types of solutions
Function
Benefits
Orthosis
Compensation of a deficient function, joint support
Pain prevention
Ergonomic cushion
Improvement of posture and comfort
Reduction of risk of pressure sores
Manual wheelchair
Mobility by manual propulsion
Maintains movement autonomy
Electric wheelchair
Robotized mobility
Increased autonomy over long distances
Ergonomic cane
Walking support
Improved balance and gait
Ergonomic pen
Facilitate writing or drawing
Maintain graphic activity despite deficits
Adapted cutlery
Facilitate eating
Less effort to hold and manipulate
Types of solutions | Function | Benefits | Orthosis | Compensation of a deficient function, joint support
| Pain prevention |
|---|---|---|
Ergonomic cushion | Improvement of posture and comfort
| Reduction of risk of pressure sores |
Manual wheelchair | Mobility by manual propulsion | Maintains movement autonomy
|
Electric wheelchair
| Robotized mobility | Increased autonomy over long distances
|
Robotic arm support | Robotized assistance for arm gestures | Compensation for strength and range |
Ergonomic cane | Walking support | Improved balance and gait |
Ergonomic pen | Facilitate writing or drawing | Maintain graphic activity despite deficits |
Adapted cutlery | Facilitate eating | Less effort to hold and manipulate |
Functional rehabilitation exercises in occupational therapy
There are no “standard” exercises in occupational therapy. Only an occupational therapist knows how to guide functional rehabilitation exercises. The exercises offered are personalized and adapted to the person’s overall capacities (mobility, pain, etc.).
Innovative technologies in neuromuscular occupational therapy
Contribution of robotic and mechatronic devices
At ORTHOPUS, we offer a range of robotic assistants that cover all arm mobility needs, with only one robotic assistant currently available: the ORTHOPUS Supporter.
Our device, the ORTHOPUS Supporter, has an orthosis available in several sizes for different morphologies. It works with two modes: FIXED mode and FREE mode.
- FIXED mode maintains a stable, fixed position to, for example, make calls or read.
- FREE mode accompanies the user’s movement, their arm is supported but not fixed.
Our shells are also customizable in 8 colors.
Artificial intelligence and human-machine interfaces
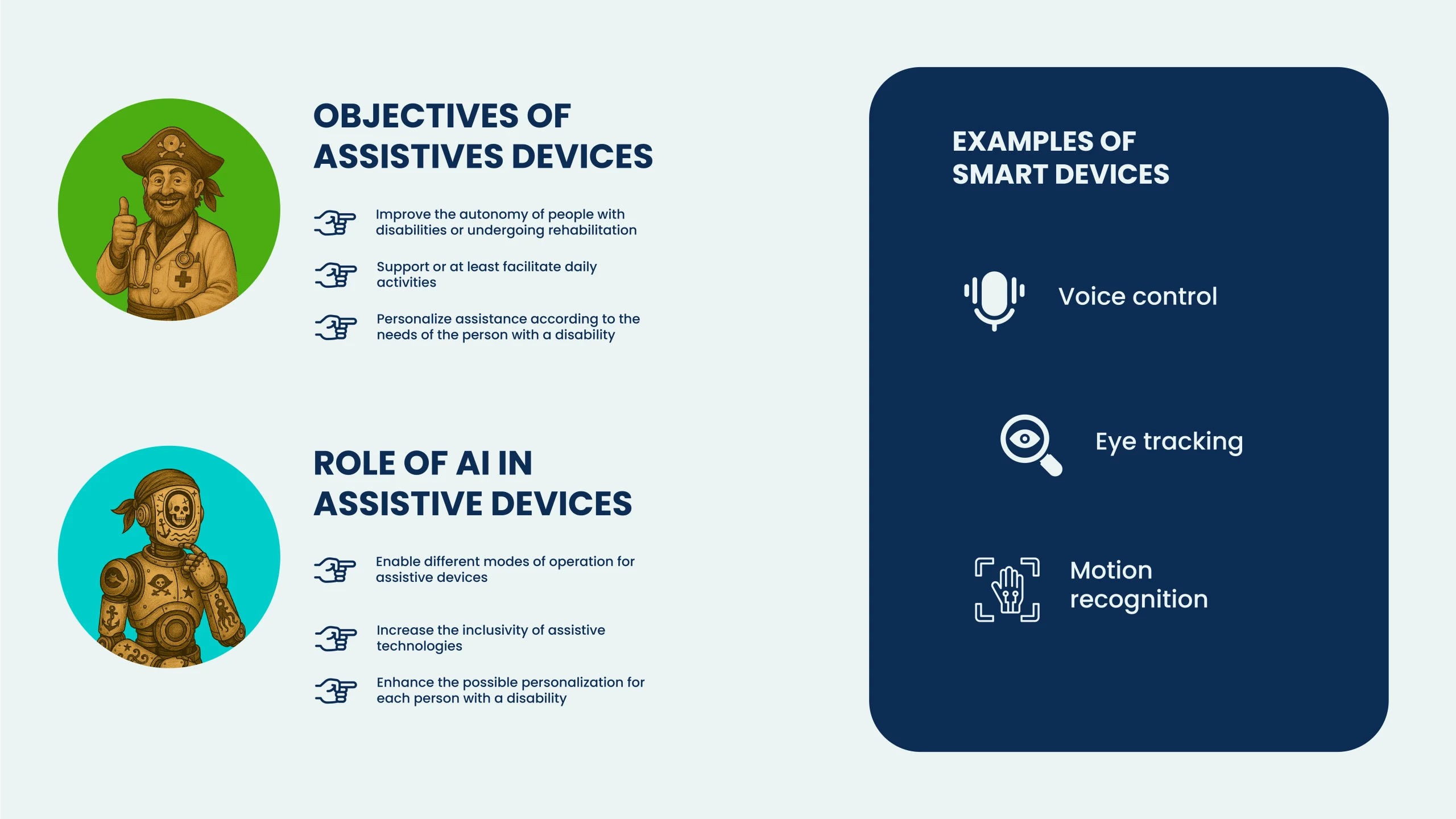
Innovations in artificial intelligence (AI) are increasingly prominent in technological assistance for people with disabilities. This occurs through three modes:
- Voice control: thanks to AI-driven voice recognition, people with disabilities can control devices remotely or without manual intervention.
- Eye-tracking: device control is enabled through eye movements, detected by an AI system.
- Movement recognition: with high-frequency sensors, this mode can move devices remotely even with almost imperceptible movements.
Impact of open-source and connected solutions
An open-source solution is an open and accessible tool to everyone (for example, code can be open-source). This means anyone can view, modify, use, and share freely, depending on the Creative Commons license.
These solutions play a key role in designing technological innovations that are accessible and adaptable to as many people as possible. Thanks to their collaborative and evolving availability, they allow the development of modular technologies adapted to each individual’s needs.
Advantages of robotic solutions for people with neuromuscular diseases
Improvement of autonomy and independence
These robotic solutions help promote autonomy and independence in everyday gestures. Users of these solutions do not need constant external assistance, thus improving their personal well-being. With these robotic solutions, they can perform their daily activities more easily.
- Eating independently: robotic arms allow food to be brought to the mouth with the user’s intention, eating at their own pace.
- Writing privately: robotic pens or smart interfaces remove the need for an intermediary to transcribe.
- Washing independently: some automated tools help perform hygiene care.
- Using a smartphone or computer independently: voice and eye controls expand possibilities without constant manual interaction with the screen or keyboard.
Reduction of fatigue and better social participation
Simon, a 23-year-old German living with Duchenne muscular dystrophy and user of the ORTHOPUS Supporter:
“I use my arm support to paint, build models, drink, and smoke. This allows me to be less dependent on my caregiver and to refocus on my hobbies.”
How to choose the right assistance solution with the help of an occupational therapist?
Importance of personalized assessment
The occupational therapist plays a central role in the process of choosing an appropriate technical solution. After an in-depth analysis of the needs, difficulties, and lifestyle of the person with a disability, They evaluate existing possibilities to recommend the most suitable solution. They may integrate devices into the assistance plan, but above all they explain how to integrate and use them daily.
Like an ophthalmologist who can prescribe glasses for reading, in certain situations, an occupational therapist recommends the use of a technological device, such as a robotic arm for eating.
Criteria to consider when choosing a device
When it comes to choosing an assistive device, several specific criteria must be considered in order to find the solution that best suits the user.
- Ergonomics: the device must be comfortable, intuitive, and adapted to the user’s body shape and abilities. Good ergonomics make the device easier to adopt and help reduce fatigue.
- Compatibility with other equipment: it is essential that the assistive technology can be easily integrated into the user’s existing technological environment (computer, wheelchair, smartphone, home automation, etc.).
- Ease of use: the interface and operation should be simple to understand and handle, so as not to add unnecessary complexity to daily life.
- Cost: the purchase price, maintenance, and update costs of the device must be taken into account, as well as available funding or reimbursement options.
- Availability of updates and technical support: reliable technical support and the ability to upgrade the device over time are key factors in ensuring its long-term use and its adaptation to the user’s evolving needs.
Choosing an appropriate assistive solution is not simply a matter of purchasing equipment. It requires a careful assessment of needs, living context, and personal goals. Support from a professional helps avoid costly mistakes and maximizes the impact of assistive devices in everyday life. Thanks to in-depth knowledge of available assistive technologies, the neuromuscular occupational therapist guides users toward the most ergonomic, scalable, and lifestyle-compatible solutions.
Frequently asked questions
What are the main missions of an occupational therapist?
When is it recommended to consult an occupational therapist?
It is advisable to consult in case of difficulties in performing daily life tasks, regardless of the cause or severity.
How long does an occupational therapy assessment last?
Sources:
- Bureau of Labor Statistics. “Occupational Therapists.” https://www.bls.gov/ooh/healthcare/occupational-therapists.htm
- BTE Technologies. “Neuromuscular Reeducation in Occupational Therapy.” https://www.btetechnologies.com/therapyspark/neuromuscular-reeducation-in-occupational-therapy/
- Wikipedia. “Neuromuscular disease.” https://en.wikipedia.org/wiki/Neuromuscular_disease
- UNRIC. “Building an Accessible Future for All: AI and the Inclusion of Persons with Disabilities.” https://unric.org/en/building-an-accessible-future-for-all-ai-and-the-inclusion-of-persons-with-disabilities/
- Wikipedia. “Occupational therapist.” https://en.wikipedia.org/wiki/Occupational_therapist
- Cleveland Clinic. “Occupational Therapist.” https://my.clevelandclinic.org/health/articles/24617-occupational-therapist
